Skin wound healing: Scientists in São Paulo, Brazil, have created an affordable anti-inflammatory hydrogel that could potentially help in managing persistent skin wounds, often observed in people with diabetes. The findings from their animal research are detailed in an article published in the Biomedicine & Pharmacotherapy journal.
The International Diabetes Federation reports that Brazil is the sixth-highest country globally in terms of diabetes prevalence. This disease, now considered an epidemic, is the fifth leading cause of death worldwide. Approximately 17.7 million Brazilians grapple daily with metabolic changes due to insufficient insulin production and function, leading to conditions like nephropathy (kidney damage), neuropathy, and hindered wound healing. It is estimated that one in five diabetics will develop chronic wounds, such as foot ulcers.
In healthy individuals, a skin injury immediately triggers a sequence of events leading to healing. Platelet aggregation manages bleeding by providing binding sites for coagulation and cell growth, followed by the creation of new blood cells and collagen accumulation. However, in diabetics, elevated blood sugar levels (hyperglycemia) boost the production of reactive oxygen species, which intensify inflammation and hinder blood vessel growth.
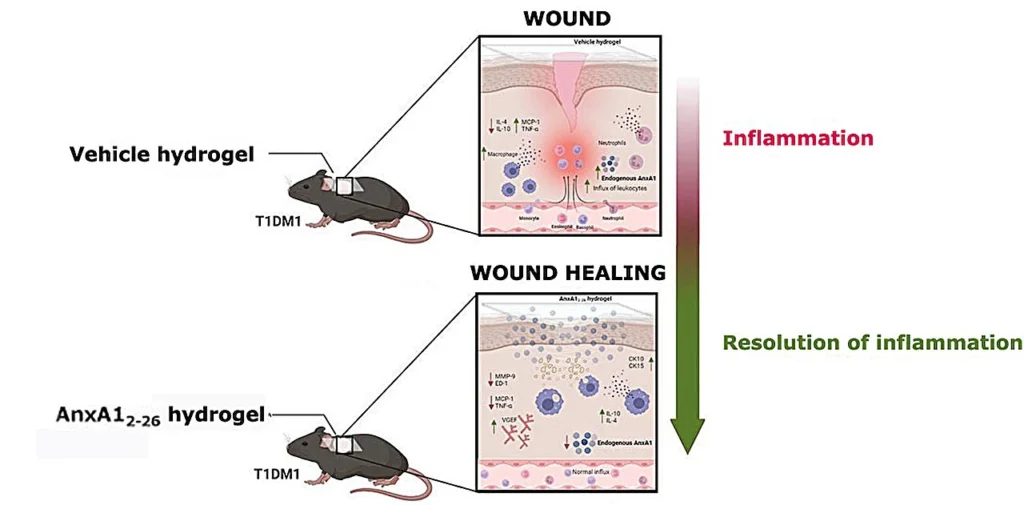
Biological hydrogels have proven effective in accelerating wound healing by providing a moist and sterile environment. In this study, researchers from São Paulo State University (UNESP) and the Federal University of São Paulo (UNIFESP) developed a formula based on annexin A1 (AnxA1), a protein known to regulate inflammation and cell proliferation, as shown in the group’s previous research. The study’s findings suggest that the hydrogel can modify the wound microenvironment and stimulate tissue regeneration.
A peptide called AnxA12–26 was added to a hydrogel and tested on mice with skin wounds and diabetes.A decrease in inflammatory cells was observed three days after wound infliction. By the 14th day, the wounds had completely healed. In contrast, the control group, which included diabetic mice treated with a hydrogel devoid of peptides, showed extended acute wound inflammation beyond the third day.
Immunohistochemical analysis showed that the tissue regenerated better. This was because the cells that make up the skin grew faster, there were fewer immune cells that cause inflammation, and there was more of a protein that helps to make new blood vessels.
The cytotoxicity test showed excellent biocompatibility, verifying the hydrogel’s safety for treating diabetic wounds. “Our hydrogel is highly absorbent, providing the ideal moisture level to promote healing, which actually happens faster than without it. It’s an effective alternative to expanding the therapeutic options for treating diabetic wounds,” said Sonia Maria Oliani, the article’s final author.
Oliani is a faculty member at UNESP’s Institute of Biosciences, Letters, and Exact Sciences (IBILCE) and UNIFESP’s Program of Graduate Studies in Functional and Structural Biology.
Researchers in São Paulo developed a hydrogel that is easy to produce and cost-effective, which are vital factors in South and Central America, where the annual cost of diabetes care exceeds USD 65.3 billion.
The product also shows potential for other applications. Currently, the researchers are investigating its efficacy in treating oral mucosal wounds.
Read also: Indian scientists find out how tissues react to wound healing



Diabetes patients’ skin wound healing may be enhanced by an inexpensive anti-inflammatory hydrogel